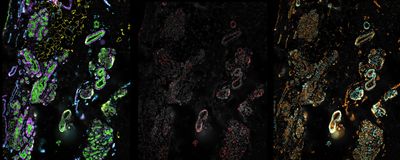
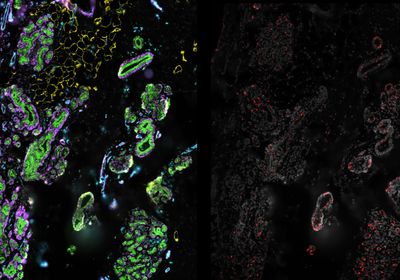
ABOVE: Breast tissue from a transgender man visualized with fluorescent probes, including one for androgen receptors (red) FLORIAN RATHS AND CEDARS SINAI MEDICAL CENTER
When transgender men transition, they may choose to take androgens—masculinizing hormones including testosterone—and undergo gender-affirming surgery. Hormone treatments affect the entire body, from redistributing fat to terminating menstrual cycles, but “we don’t really know how much androgens work on the molecular level,” says Florian Raths, a researcher in single cell technology development who currently works as a consultant for Vevo Therapeutics.
That’s why, for a study published March 8 in Cell Genomics, Raths and colleagues pinpointed the molecular events that take place in breast tissue brought about by androgens. The changes lead to breast cells that resemble those seen in cisgender men, including the suppression of genes linked to breast cancer.
“This study is a “tour de force” showing the molecular effects of androgen therapy in the breast tissue of trans men,” Michael Irwig, an endocrinologist at Beth Israel Deaconess Medical Center in Massachusetts, who was not involved in the study, writes in an email to The Scientist. “The breadth and depth of the analyses are quite impressive,” he adds.
The work began when Raths was working on his PhD at Cedars Sinai Medical Center in California. There, he was presented with the rare opportunity to study nondiseased human samples. “Often, tissues are collected as part of a cancer surgery, or after some other illness,” he explains, but being situated in West Hollywood—a hub for the LGBTQ+ community—the hospital performs a number of gender-affirming surgeries, enabling Raths to collect the tissues needed to study the effects of androgens in healthy cells.
See “Are the Brains of Transgender People Different from Those of Cisgender People?”
The team analyzed breast tissue from nine transgender men collected during gender-affirming surgery and compared it to tissue obtained from nine cisgender women during cosmetic surgery. By extracting the nuclei from tens of thousands of individual cells and sequencing their RNA, they could identify genetic changes triggered by hormone therapy.
Breast cells from transgender men expressed fewer genes, suggesting that androgen treatment silences gene expression in the tissue. “The whole breast seems to be less active,” says Simon Knott, a computational biologist at Cedars Sinai Medical Center who led the research.
Hormone treatment also induced gene expression patterns that are typically seen in cisgender men. For instance, the researchers noted the upregulation of a gene called CUX2, a transcription factor that is strongly expressed in the prostate and other cis-male tissues.
While changes in gene expression and chromatin architecture were detected across all types of breast cells, only a fraction of these cells possess the receptor to detect androgens. That suggests the androgen-sensitive cells then communicate to neighbors through paracrine signaling, inducing changes across the whole tissue, say the researchers.
The work characterizes the complexity of androgen signaling at a resolution that has never been seen before,” says Étienne Audet-Walsh, an endocrinologist at Laval University in Canada, who was not involved in the study. “There is depth in their analysis,” he adds.
Hormone therapy for cancer?
In addition to detailing how androgens affect breast tissues, the work also sheds light on the possible use of androgens in cancer therapy. When the team documented the different types of breast cells in their samples, they noted a reduction in cells involved in estrogen signaling in the transgender men’s tissues, supporting androgens’ known antagonistic effects against estrogen. Estrogen signaling plays a role in the growth of some breast cancers, and androgens have been previously fingered as a potential therapy. Indeed, the risk of breast cancer plummets when transgender men start androgen treatment, and the new study showed that androgen therapy downregulates genes that are usually activated in estrogen-driven breast cancers.
See “While the Body Rests, Breast Cancer Spreads More Aggressively”
Immune system changes may also contribute to androgen’s antitumor effect, says Knott. The team documented more immune cells, specifically CD4 T-cells, in the breast tissue of transgender men, indicating improved immune surveillance to ward off cancer cells, he says.
Clinical trials are already underway to test the effectiveness of androgens in treating breast cancer. Similar therapies could also be used as a preventative strategy in people at high risk of the condition, say the researchers. But others urge caution. As the study shows, “playing with hormones has a lot of different changes, and we don’t yet know their long-term impact,” says Audet-Walsh.